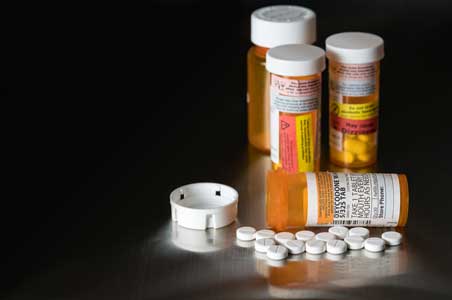
Rule # 1 For Many Professional Guardians
If they're too much work—Drug'em
By Romona Paden
The training manual for the education of a professional guardian states that it is the guardian’s responsibility to find their own clients (wards). The need for financing to support the professional guardianship business makes a target of every elderly American with anything of value. Jacqueline Scott ended up right in the center of one of those bull’s-eyes.
Many professional guardians have far too many wards to attend to. Frequently, the wards are located in areas many miles from each other, and the administration of drugs allows the guardians to simply warehouse these elderly victims. Most nonprofessional guardians are loving, caring individuals. The same can be said for many professional guardians. However, some of the worst and most cruel elder abusers are professional guardians. What Kathy Dunn witnessed happening to her elderly mother Jacqueline amounted to chemical restraint—the use of pharmaceuticals to restrict a patient’s freedom of movement or to sedate a patient.
In the last years of her life, Jacqueline spoke very few words. Confined to a windowless room in a nursing home facility, the once independent and vital woman found herself trapped in a pharmacological stupor. Measuring a petite 5’2” and weighing only 82 pounds on entering the facility, Scott’s caregivers put her on a daily, steady cocktail of Xanax and Lexapro punctuated with months-long dosing of various forms of Ambien as well as Zyprexa and Temazepam. She regularly sat totally unconscious in her straight-backed chair.
 She was deficient in both D-3 and B-12, and no effort was made to include food high in these vitamins in Scott’s meals, nor were nutritional supplements provided. Her tiny frame diminished to a mere 4’9” and just a hair over 70 pounds by the time she died.
She was deficient in both D-3 and B-12, and no effort was made to include food high in these vitamins in Scott’s meals, nor were nutritional supplements provided. Her tiny frame diminished to a mere 4’9” and just a hair over 70 pounds by the time she died.
This brutal nearly four-year ordeal arose from an unrequested, unneeded, and unwanted guardianship, says her daughter. Scott’s guardian hyped the mild dementia of her charge in order to justify the move into a nursing home facility. Her next step was to develop a source of funds to cover her guardianship fees and pay her lawyer. As is often the case, this was handily dealt with by selling Scott’s mortgage-free home.
“My mother was held against her will in a nursing home that was a two-hour round trip from me,” says Dunn of the period from late October 2010 until her mother’s death in August 2015.
“Chemical restraint is inadvisable for elderly patients outside of a psychiatric ward,” says Alethea Fleming, a naturopathic doctor focused on gerontology, from her Vital Aging Clinic in Anacortes, Washington. While Fleming doesn’t offer comment directly on patients who are not in her care, she keenly acknowledges the pervasiveness of an overmedicated senior population.
“Older patients tend to really get the shaft,” says Fleming.
According to AgingCare.com, “While nursing home regulations have come a long way, the past practice of chemical sedation continues to tarnish the industry’s reputation and factors into family discussions re: long-term health care.”
 In the case of Harvey Whitten, a veteran who acted as a medic during the Korean War, the spiral into drug-induced confusion began with a stroke he suffered in late summer of 2010 and a diagnosis of vascular dementia when he was 80 years old. The situation initially beamed a silver lining as Whitten moved from his home in California to live with his lifelong friend Robert Sprau in Montgomery County, Pennsylvania. By early 2011, however, the bright side quickly began to tarnish.
In the case of Harvey Whitten, a veteran who acted as a medic during the Korean War, the spiral into drug-induced confusion began with a stroke he suffered in late summer of 2010 and a diagnosis of vascular dementia when he was 80 years old. The situation initially beamed a silver lining as Whitten moved from his home in California to live with his lifelong friend Robert Sprau in Montgomery County, Pennsylvania. By early 2011, however, the bright side quickly began to tarnish.
Through court hearings, a Montgomery County judge appointed guardianship responsibilities to a local attorney. Although the judge also named Sprau, Whitten’s longtime friend and new roommate, and Whitten’s adored niece, Cosmas Skaife, as co-guardians, Sprau became ill and died in the fall of 2012, and the legal apparatchik systematically minimized Skaife’s authority in overseeing her uncle’s care. With this, Whitten’s best interest, no longer in the hands of a person who loved him, quickly fell by the wayside.
Skaife lobbied for the opportunity to bring her Uncle Harvey to live in a facility near her home in Madison, Wisconsin. At every turn, her efforts were undercut by a legal system that often seemed to exist solely to serve institutional interests over those of the individual and family.
While leaving him without his glasses, his hearing aid, or his dentures, the guardian, having control over Whitten’s money and assets, charged for guitar music and singing lessons conducted by a friend of the guardian at a cost of $125 per hour as well as so-called pet therapy (though he’d never owned a pet).
Despite a monthly income of more than $13,000, the guardian contended additional costs associated with Whitten’s care made the cash flow insufficient. To cover his care, according to Skaife’s documentation on the matter, the guardian accessed his more than $4 million in savings.
Besides attacking his financial health, Whitten’s guardians likewise demonstrated disregard for his physical health. He was chemically restrained by a daily dose of 5 milligrams of Haldol, an antipsychotic drug used to treat mental and mood disorders like schizophrenia and acute psychosis.
“That’s huge,” says Panayiotis Tsitouras, an MD and associate professor at the University of Oklahoma. “No, that’s unacceptable.”
Speaking in a general sense, Tsitouras says the common dosage of Haldol for elderly patients who “experience real problems with anxiety, sleep, or pain” ranges from .5 milligrams to 1 milligram. In terms of the overprescription of medicines for the elderly, Tsitouras says, “Hopefully society is becoming more sensitive to those issues.”
Whitten died in April 2016.
Every day of the year, 10,000 baby boomers turn 65, and this will continue for years. Contrary to claims of many, tough laws governing and punishing guardians’ behavior will not discourage good people from becoming guardians, but what those laws will do is discourage the bad apples. In addition, families must make long-term health care plans well in advance of old age.
One factor that can connect directly to the heart of the polypharmacy issue is the many seniors who have spent years on pharmaceuticals without any modifications in dosing. Considering that the liver, kidneys, and other organs of elimination become more sluggish with age, the problem becomes even more pronounced among the senior population. What’s more, patients aged 80-plus “don’t ask questions,” Fleming says. The combination of all these factors means that potential damage due to overmedication reaches exponential proportions.
You might consider, before jumping right into heavy drugs, first trying a naturopathic physician (ND) whose work centers on a holistic approach to patient care. While trained to carry out many of the same approaches as allopathic practitioners and licensed to prescribe traditional pharmaceuticals, NDs manage chronic disease and acute conditions through herbal medicine, nutrition, homeopathy, and therapeutic physical techniques. Alethea Fleming says that her practice focuses on the foundations of health “taking a decidedly conservative approach in prescribing medication” and “treating the whole person using the least forceful intervention first.”
“Dose low and go slow,” serves as her mantra.
“I listen to them,” Fleming says. Carving out meaningful discussions with patients allows her to garner the kind of depth and breadth of information necessary to guide patient healthcare to optimize health and to treat illness. Vital in this is gaining the full picture on pharmaceuticals. It not unheard of, for instance, to come across a patient in retirement years who’s still taking high blood pressure meds prescribed decades prior while working a high-stress job.
Another critical element in establishing patient background includes determining situational circumstances around family proximity. This is an important topic as “far-flung families” mean some patients lack a strong support network.
Still another element playing into the overmedication of seniors, says Fleming, centers on the lack of continuity in care. Seniors using a piecemeal approach to pharmacies and providers also plays into the problem.
Unfortunately, the medical community counts only around 6,000 naturopaths in its ranks across the United States. Just over half the states and territories in the nation (23 of them) extend licensing to NDs—others must be encouraged to do so, and Medicare must begin covering these visits. As a starting point, it is less expensive and a safer place to begin.
The government must do a better job of monitoring abusive drug administration.
Somewhat surprisingly, the U.S. Department of Health and Human Services recorded only 74 complaints around chemical restraint among individuals living in long-term care facilities, according to Kelly Mack, a public affairs specialist with the Administration for Community Living that operates within HHS. That number, reported for 2016, comes through states’ long-term care ombudsman programs, which are designed to resolve problems around individuals’ health, safety, welfare, and rights. All one needs to see is the mountain of letters coming into the National Association to Stop Guardian Abuse to know this number is way off.
“Another complaint code for medications-administration, organization,” Mack writes in an email, “has a larger amount of complaints but is not pertaining just to inappropriate drugging, so we have nothing more detailed.”
In an interview with PBS, Maristela Garcia, a physician and director of the geriatric medication unit at UCLA Medical Center, summed up the result of guardians and nursing homes using medication as a tool to control, doctors overprescribing to placate the complaints of their aging patients, and seniors self-medicating: “This is America’s other drug problem—polypharmacy, and it’s huge!”
Note:
The picture on the left target is Lynn Sayler’s mother Retta, on the Right Marie Claire Conners’ mother Grace. Both stories can be seen in the documentary The Unforgivable Truth at http://vimeo.com/user5231742/uft.
Mercedes Kibbee, whose story is also told in The Unforgivable Truth, was so addicted to the excessive drugs being pumped into her that, when her daughter realized what was happening and changed her doctor, Mercedes went through a very painful drug withdrawal that lasted for more than a week.
















 The thing I miss the most about being a younger person is supple skin. The face that looks back at me in the mirror has all the same features, but the skin doesn’t seem to fit around them quite as nicely as it used to. There is a little excess around the chin and wrinkles around the eyes that look like they don’t exactly know what to do with themselves.
The thing I miss the most about being a younger person is supple skin. The face that looks back at me in the mirror has all the same features, but the skin doesn’t seem to fit around them quite as nicely as it used to. There is a little excess around the chin and wrinkles around the eyes that look like they don’t exactly know what to do with themselves.

 She was deficient in both D-3 and B-12, and no effort was made to include food high in these vitamins in Scott’s meals, nor were nutritional supplements provided. Her tiny frame diminished to a mere 4’9” and just a hair over 70 pounds by the time she died.
She was deficient in both D-3 and B-12, and no effort was made to include food high in these vitamins in Scott’s meals, nor were nutritional supplements provided. Her tiny frame diminished to a mere 4’9” and just a hair over 70 pounds by the time she died. In the case of Harvey Whitten, a veteran who acted as a medic during the Korean War, the spiral into drug-induced confusion began with a stroke he suffered in late summer of 2010 and a diagnosis of vascular dementia when he was 80 years old. The situation initially beamed a silver lining as Whitten moved from his home in California to live with his lifelong friend Robert Sprau in Montgomery County, Pennsylvania. By early 2011, however, the bright side quickly began to tarnish.
In the case of Harvey Whitten, a veteran who acted as a medic during the Korean War, the spiral into drug-induced confusion began with a stroke he suffered in late summer of 2010 and a diagnosis of vascular dementia when he was 80 years old. The situation initially beamed a silver lining as Whitten moved from his home in California to live with his lifelong friend Robert Sprau in Montgomery County, Pennsylvania. By early 2011, however, the bright side quickly began to tarnish.
 Three married women are forced into an instant-oatmeal life of disorganized crime to pay back the debts that their underworldly husbands "owed" when they were killed during a botched armed robbery.
Three married women are forced into an instant-oatmeal life of disorganized crime to pay back the debts that their underworldly husbands "owed" when they were killed during a botched armed robbery.

 This desert country lies between Iran, Afghanistan, and the Caspian Sea. Turkmenistan is famous for cotton textiles, hand-woven red Turkmen carpets, and metalworking. The ancient city of Merv nearby (now in ruins) was once one of the greatest Islamic cities in the world and a crucial stopping point on the Silk Road.
This desert country lies between Iran, Afghanistan, and the Caspian Sea. Turkmenistan is famous for cotton textiles, hand-woven red Turkmen carpets, and metalworking. The ancient city of Merv nearby (now in ruins) was once one of the greatest Islamic cities in the world and a crucial stopping point on the Silk Road.



 As we have just begun, we have not yet received any letters. I certainly hope that you will write to us: tell us about your experience with Financial Elder Abuse or Involuntary Guardianship. We will also be looking for people to interview for our monthly video and lovely photographs for our cover.
As we have just begun, we have not yet received any letters. I certainly hope that you will write to us: tell us about your experience with Financial Elder Abuse or Involuntary Guardianship. We will also be looking for people to interview for our monthly video and lovely photographs for our cover.